
Summary
Clostridium perfringens alpha toxin is a toxin produced by the bacterium Clostridium perfringens (C. perfringens) and is responsible for gas gangrene and myonecrosis in infected tissues. The toxin also possesses hemolytic activity.
| alpha toxin | |||||||
|---|---|---|---|---|---|---|---|
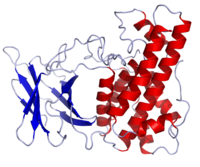 Crystal structure of Clostridium perfringens alpha toxin | |||||||
| Identifiers | |||||||
| Organism | |||||||
| Symbol | plc | ||||||
| Alt. symbols | phospholipase C, CPE0036, Zn_dep_PLPC | ||||||
| Entrez | 988262 | ||||||
| PDB | 1CA1 1KHO, 1GYG, 1QM6, 1QMD, 1KHO, 1GYG, 1QM6, 1QMD | ||||||
| UniProt | P0C216 | ||||||
| Other data | |||||||
| EC number | 3.1.4.3 | ||||||
| |||||||
Clinical significance edit
This toxin has been shown to be the key virulence factor in infection with C. perfringens; the bacterium is unable to cause disease without this toxin.[1] Further, vaccination against the alpha toxin toxoid protects mice against C. perfringens gas gangrene.[2] As a result, knowledge about the function of this particular protein greatly aids understanding of myonecrosis.[citation needed]
Structure and homology edit
The alpha toxin has remarkable similarity to toxins produced by other bacteria as well as natural enzymes. There is significant homology with phospholipase C enzymes from Bacillus cereus, C. bifermentans, and Listeria monocytogenes.[3] The C terminal domain shows similarity with non-bacterial enzymes such as pancreatic lipase, soybean lipoxygenase, and synaptotagmin I.[4]
The alpha toxin is a zinc metallophospholipase, requiring zinc for activation. First, the toxin binds to a binding site on the cell surface. The C-terminal C2-like PLAT domain binds calcium and allows the toxin to bind to the phospholipid head-groups on the cell surface. The C-terminal domain enters the phospholipid bilayer. The N-terminal domain has phospholipase activity. This property allows hydrolysis of phospholipids such as phosphatidyl choline, mimicking endogenous phospholipase C. The hydrolysis of phosphatidyl choline produces diacylglycerol, which activates a variety of second messenger pathways. The end-result includes activation of arachidonic acid pathway and production of thromboxane A2, production of IL-8, platelet-activating factor, and several intercellular adhesion molecules. These actions combine to cause edema due to increased vascular permeability.[3]
See also edit
References edit
- ^ Awad, M.M.; Bryant, A.E.; Stevens, D.L. & Rood, J.I. (1995). "Virulence studies on chromosomal alpha-toxin and alpha-toxin mutants constructed by allelic exchange provide genetic evidence for the essential role of alpha-toxin in Clostridium perfringens-mediated gas gangrene". Mol Microbiol. 15 (2): 191–202. doi:10.1111/j.1365-2958.1995.tb02234.x. PMID 7746141.
- ^ Williamson ED, Titball RW (1993). "A genetically engineered vaccine against the alpha-toxin of Clostridium perfringens also protects mice against experimental gas gangrene". Vaccine. 11 (12): 1253–1258. doi:10.1016/0264-410X(93)90051-X. PMID 8256506.
- ^ a b Sakurai J, Nagahama M, Oda M (2004). "Clostridium perfringens Alpha-Toxin: Characterization and Mode of Action". J Biochem. 136 (5): 569–574. doi:10.1093/jb/mvh161. PMID 15632295.
- ^ Naylor CE, Eaton JT, Howells A, et al. (1998). "Structure of the key toxin in gas gangrene". Nature Structural & Molecular Biology. 5 (8): 738–746. doi:10.1038/1447. PMID 9699639.


