
Summary
Tomotherapy is a type of radiation therapy treatment machine.[1][2][3] In tomotherapy a thin radiation beam is modulated as it rotates around the patient, while they are moved through the bore of the machine. The name comes from the use of a strip-shaped beam, so that only one “slice” (Greek prefix “tomo-”) of the target is exposed at any one time by the radiation. The external appearance of the system and movement of the radiation source and patient can be considered analogous to a CT scanner (computed tomography), which uses lower doses of radiation for imaging. Like a conventional machine used for X-ray external beam radiotherapy (often referred to as a linear accelerator or linac, their main component), a linear accelerator generates the radiation beam, but the external appearance of the machine, the patient positioning, and treatment delivery is different. Conventional linacs do not work on a slice-by-slice basis but typically have a large area beam which can also be resized and modulated.[4][5][6]
| Tomotherapy | |
|---|---|
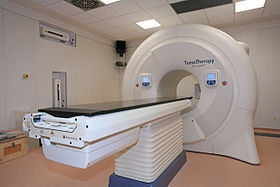 Tomotherapy Hi Art machine | |
| Other names | Helical tomotherapy |
| Specialty | oncology |
General principles edit
The treatment field's length (the width of the radiation slice) is adjustable using collimator jaws. In static-jaw delivery, the field length remains constant during a treatment. In dynamic-jaw delivery, the field length changes so that it begins and ends at its minimum setting.
Tomotherapy treatment times vary compared to normal radiation therapy treatment times. Tomotherapy treatment times can be as low as 6.5 minutes for common prostate treatment,[7] excluding extra time for imaging. Modern tomotherapy and conventional linac systems incorporate one or both of megavoltage X-ray or kilovoltage X-ray imaging systems, enabling image-guided radiation therapy (IMRT). In tomotherapy, images are acquired in a very similar manner to a CT scanner, thanks to their closely related design.[8][9][10]
There are few head-to-head comparisons of tomotherapy and other IMRT techniques, however there is some evidence that a conventional linac using VMAT can provide faster treatment whereas tomotherapy is better able to spare surrounding healthy tissue while delivering a uniform dose.[11][12][13]
Helical delivery edit
In helical tomotherapy, the linac rotates on its gantry at a constant speed while the beam is delivered; so that from the patient's perspective, the shape traced out by the linac is helical.[14]
While helical tomotherapy can treat very long volumes without a need to abut fields in the longitudinal direction, it does display a distinct artifact due to "thread effect"[15] when treating non-central tumors. Thread effect can be suppressed during planning through good pitch selection.
Fixed-angle delivery edit
Fixed-angle tomotherapy uses multiple tomotherapy beams, each delivered from a separate fixed gantry angle, in which only the couch moves during beam delivery. This is branded as TomoDirect, but has also been called topotherapy.[16]
The technology enables fixed beam treatments by moving the patient through the machine bore while maintaining specified beam angles.
Clinical considerations edit
Lung cancer, head and neck tumors, breast cancer, prostate cancer, stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are some examples of treatments commonly performed using tomotherapy.[17][18][19]
In general, radiation therapy (or radiotherapy) has developed with a strong reliance on homogeneity of dose throughout the tumor. Tomotherapy embodies the sequential delivery of radiation to different parts of the tumor which raises two important issues. First, this method is known as "field matching" and brings with it the possibility of a less-than-perfect match between two adjacent fields with a resultant hot and/or cold spot within the tumor. The second issue is that if the patient or tumor moves during this sequential delivery, then again, a hot or cold spot will result. The first problem is reduced by use of a helical motion, as in spiral computed tomography.[20]
Some research has suggested tomotherapy provides more conformal treatment plans and decreased acute toxicity.[21]
Non-helical static beam techniques such as IMRT and TomoDirect are well suited to whole breast radiation therapy. These treatment modes avoid the low-dose integral splay and long treatment times associated with helical approaches by confining dose delivery to tangential angles.[22][23][24]
This risk is accentuated in younger patients with early-stage breast cancer, where cure rates are high and life expectancy is substantial.[24]
Static beam angle approaches aim to maximize the therapeutic ratio by ensuring that the tumor control probability (TCP) significantly outweighs the associated normal tissue complication probability (NTCP).[25][26][27]
History edit
The tomotherapy technique was developed in the early 1990s at the University of Wisconsin–Madison by Professor Thomas Rockwell Mackie and Paul Reckwerdt.[28] A small megavoltage x-ray source was mounted in a similar fashion to a CT x-ray source, and the geometry provided the opportunity to provide CT images of the body in the treatment setup position. Although original plans were to include kilovoltage CT imaging, current models use megavoltage energies. With this combination, the unit was one of the first devices capable of providing modern image-guided radiation therapy (IGRT).[20]
The first implementation of tomotherapy was the Corvus system developed by Nomos Corporation, with the first patient treated in April 1994.[29][17] This was the first commercial system for planning and delivering intensity modulated radiation therapy (IMRT). The original system, designed solely for use in the brain, incorporated a rigid skull-based fixation system to prevent patient motion between the delivery of each slice of radiation. But some users [30] eschewed the fixation system and applied the technique to tumors in many different parts of the body.
Mobile tomotherapy edit
Due to their internal shielding and small footprint, TomoTherapy Hi-Art and TomoTherapy TomoHD treatment machines were the only high energy radiotherapy treatment machines used in relocatable radiotherapy treatment suites. Two different types of suites were available: TomoMobile developed by TomoTherapy Inc. which was a moveable truck; and Pioneer, developed by UK-based Oncology Systems Limited. The latter was developed to meet the requirements of UK and European transport law requirements and was a contained unit placed on a concrete pad, delivering radiotherapy treatments in less than five weeks.[31][32]
See also edit
References edit
- ^ Mayles, Philip; Nahum, Alan; Rosenwald, Jean-Claude, eds. (2007). Handbook of radiotherapy physics theory and practice. Boca Raton: CRC Press. p. 969. ISBN 9781420012026.
- ^ Colligan, S J; Mills, J (2012). "Beam therapy equipment". In Sibtain, Amen; Morgan, Andrew; MacDougall, Niall (eds.). Radiotherapy in practice : physics for clinical oncology. Oxford: Oxford University Press. doi:10.1093/med/9780199573356.001.0001. ISBN 9780199573356.
- ^ Fenwick, John D.; Tomé, Wolfgang A.; Soisson, Emilie T.; Mehta, Minesh P.; Rock Mackie, T. (October 2006). "Tomotherapy and Other Innovative IMRT Delivery Systems". Seminars in Radiation Oncology. 16 (4): 199–208. doi:10.1016/j.semradonc.2006.04.002. PMID 17010902.
- ^ Mallick, Supriya; Rath, Goura K.; Benson, Rony (25 November 2019). Practical Radiation Oncology. Springer Nature. p. 69. ISBN 978-981-15-0073-2.
- ^ Beavis, A W (April 2004). "Is tomotherapy the future of IMRT?". The British Journal of Radiology. 77 (916): 285–295. doi:10.1259/bjr/22666727. PMID 15107318.
- ^ Bailat, Claude J; Baechler, Sébastien; Moeckli, Raphael; Pachoud, Marc; Pisaturo, Olivier; Bochud, François O (1 August 2011). "The concept and challenges of TomoTherapy accelerators" (PDF). Reports on Progress in Physics. 74 (8): 086701. Bibcode:2011RPPh...74h6701B. doi:10.1088/0034-4885/74/8/086701. S2CID 53124638.
- ^ Piotrowski, T; et al. (June 2014). "Tomotherapy: implications on daily workload and scheduling patients based on three years' institutional experience". Technology in Cancer Research & Treatment. 13 (3): 233–42. doi:10.7785/tcrt.2012.500374. PMID 24066951.
- ^ Hayat, M. A. (21 November 2007). Cancer Imaging: Instrumentation and Applications. Academic Press. p. 28. ISBN 978-0-08-055376-4.
- ^ Cai, Jing; Chang, Joe Y.; Yin, Fang-Fang (18 September 2017). Principles and Practice of Image-Guided Radiation Therapy of Lung Cancer. CRC Press. p. 144. ISBN 978-1-4987-3678-7.
- ^ Wang, Brian; Yang, Jun (December 2022). "New technologies and machines for stereotactic radiation therapy". Precision Radiation Oncology. 6 (4): 321–327. doi:10.1002/pro6.1180.
- ^ "VMAT vs. Tomotherapy". Imaging Technology News. 2010-06-02. Retrieved 6 June 2016.
- ^ Rao, M.; et al. (November 2009). "Evaluation of Arc-based Intensity Modulated Radiotherapy for Head and Neck Cancer". International Journal of Radiation Oncology, Biology, Physics. 75 (3): S419. doi:10.1016/j.ijrobp.2009.07.959.
- ^ Oliver, Michael; et al. (15 November 2009). "Comparing planning time, delivery time and plan quality for IMRT, RapidArc and Tomotherapy". Journal of Applied Clinical Medical Physics. 10 (4): 117–131. doi:10.1120/jacmp.v10i4.3068. PMC 5720582. PMID 19918236.
- ^ Darafsheh, Arash (8 March 2021). Radiation Therapy Dosimetry: A Practical Handbook. CRC Press. p. 325. ISBN 978-1-351-00537-1.
- ^ Kissick, M. W.; Fenwick, J.; James, J. A.; et al. (May 2005). "The helical tomotherapy thread effect". Medical Physics. 32 (5): 1414–1423. Bibcode:2005MedPh..32.1414K. doi:10.1118/1.1896453. PMID 15984692.
- ^ Gonzalez, Victor J.; Buchholz, Daniel J.; Langen, Katja M.; Olivera, Gustavo H.; Chauhan, Bhavin; Meeks, Sanford L.; Ruchala, Kenneth J.; Haimerl, Jason; Lu, Weiguo; Kupelian, Patrick A. (2006). "Evaluation of two tomotherapy-based techniques for the delivery of whole-breast intensity-modulated radiation therapy". International Journal of Radiation Oncology, Biology, Physics. 65 (1). Elsevier BV: 284–290. doi:10.1016/j.ijrobp.2005.12.044. ISSN 0360-3016. PMID 16618583.
- ^ a b Woo, Shiao Y.; et al. (June 1996). "A comparison of intensity modulated conformal therapy with a conventional external beam stereotactic radiosurgery system for the treatment of single and multiple intracranial lesions". International Journal of Radiation Oncology, Biology, Physics. 35 (3): 593–597. doi:10.1016/S0360-3016(96)80023-X. PMID 8655384.
- ^ Cherry, Pam; Duxbury, Angela, eds. (2009). Practical radiotherapy : physics and equipment (2nd ed.). Chichester: Wiley-Blackwell. p. 210. ISBN 9781405184267.
- ^ Peñagarícano, José A; et al. (2006). "Dosimetric comparison of Helical Tomotherapy and Gamma Knife Stereotactic Radiosurgery for single brain metastasis". Radiation Oncology. 1 (1): 26. doi:10.1186/1748-717X-1-26. PMC 1557668. PMID 16887031.
- ^ a b Mackie, T R (7 July 2006). "History of tomotherapy". Physics in Medicine and Biology. 51 (13): R427–R453. doi:10.1088/0031-9155/51/13/R24. PMID 16790916. S2CID 31523227.
- ^ Yu, Mina; et al. (2013). "A comparison of dosimetric parameters between tomotherapy and three-dimensional conformal radiotherapy in rectal cancer". Radiation Oncology. 8 (1): 181. doi:10.1186/1748-717X-8-181. PMC 3721992. PMID 23866263.
- ^ Squires M, Hu Y, Byrne M, et al. Static beam tomotherapy as an optimisation method in whole breast radiation therapy (WBRT). J Med Radiat Sci, http://onlinelibrary.wiley.com/doi/10.1002/jmrs.232/abstract
- ^ Goddu SM, Chaudhari S, Mamalui-Hunter M, et al. Helical tomotherapy planning for left-sided breast cancer patients with positive lymph nodes: Comparison to conventional multiport breast technique. Int J Radiat Oncol Biol Phys 2009; 73: 1243–51.
- ^ a b Stovall, Marilyn; Smith, Susan A.; Langholz, Bryan M.; Boice, John D.; Shore, Roy E.; et al. (2008). "Dose to the Contralateral Breast From Radiotherapy and Risk of Second Primary Breast Cancer in the WECARE Study". International Journal of Radiation Oncology, Biology, Physics. 72 (4). Elsevier BV: 1021–1030. doi:10.1016/j.ijrobp.2008.02.040. ISSN 0360-3016. PMC 3782859. PMID 18556141.
- ^ Franco P, Catuzzo P, Cante D, et al. TomoDirect: An efficient means to deliver radiation at static angles with tomotherapy. Tumori 2011; 97: 498–502.
- ^ [better source needed]
- ^ Murai, Taro; Shibamoto, Yuta; Manabe, Yoshihiko; Murata, Rumi; Sugie, Chikao; Hayashi, Akihiro; Ito, Hiroya; Miyoshi, Yoshihito (2013-03-21). "Intensity-modulated radiation therapy using static ports of tomotherapy (TomoDirect): comparison with the TomoHelical mode". Radiation Oncology. 8 (1). Springer Science and Business Media LLC: 68. doi:10.1186/1748-717x-8-68. ISSN 1748-717X. PMC 3643840. PMID 23517931.
- ^ Holmes, Timothy W.; et al. (June 2008). "Stereotactic Image-Guided Intensity Modulated Radiotherapy Using the HI-ART II Helical Tomotherapy System". Medical Dosimetry. 33 (2): 135–148. doi:10.1016/j.meddos.2008.02.006. PMID 18456165.
- ^ Mackie, T. Rockwell; Balog, John; Ruchala, Ken; et al. (January 1999). "Tomotherapy". Seminars in Radiation Oncology. 9 (1): 108–117. doi:10.1016/S1053-4296(99)80058-7. PMID 10196402.
- ^ Squires, Matthew; Hu, Yunfei; Byrne, Mikel; Archibald-Heeren, Ben; Cheers, Sonja; Bosco, Bruno; Teh, Amy; Fong, Andrew (2017-06-04). "Static beam tomotherapy as an optimisation method in whole-breast radiation therapy (WBRT)". Journal of Medical Radiation Sciences. 64 (4). Wiley: 281–289. doi:10.1002/jmrs.232. ISSN 2051-3895. PMC 5715293. PMID 28580762.
- ^ "Radiation Therapy on the Road". Imaging Technology News. 2010-04-19. Retrieved 6 June 2016.
- ^ "OSL launches Pioneer relocatable radiotherapy suite". medicalphysicsweb.org. Retrieved 6 June 2016.


